EXTREMITY TEAM
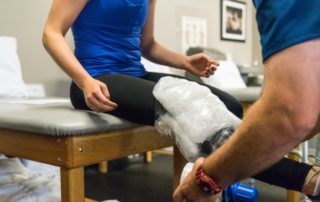
The extremity team at Physio Pro consists of physical therapists, and certified strength and conditioning specialists. These clinicians are well versed in the treatment of non-operative and post-operative orthopedic conditions of the shoulder, elbow, wrist, hip, knee, ankle and feet. These therapist are trained to utilize a variety of treatment options including manual therapy, dry needling, instrument assisted soft tissue mobilization, functional strengthening and the selective functional movement assessment (SFMA).
The therapists on the extremity team hold prominent post graduate training/certifications. These advance credentials include:
- Orthopedic Clinical Specialist (OCS): Board certification from the American Board of Physical Therapy Specialties
- Sports Clinical Specialist (SCS): Board certification from the American Board of Physical Therapy Specialties
- Certified Functional Dry Needling Practitioners
- Certified Strength and Conditioning Specialists
- Certified Functional Movement Specialists (FMS)
Manual Therapy
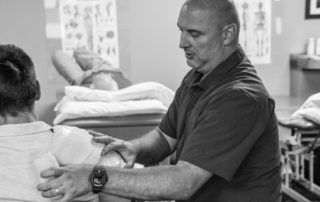
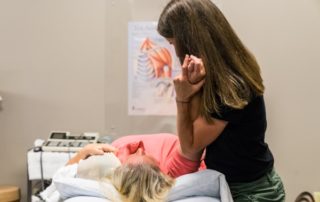
Manual Therapy is defined as a clinical approach utilizing skilled and highly specific hands-on techniques including, for example, manipulation and mobilization. A physical therapist may use these techniques to aid in diagnosing and treating soft tissues and joint structures for the purpose of:
- modulating pain
- increasing range of motion (ROM)
- reducing or eliminating soft tissue inflammation
- inducing relaxation
- improving contractile and non-contractile tissue repair, extensibility, and/or stability
- facilitating movement
- improving function
Every movement in our joints consists of a roll component and a glide component. When we start to notice mechanical pain in certain joints, we often find that there is a significant discrepancy between the rolling and gliding component within that joint. Overall range of motion can be significantly limited due to a loss of the gliding component of that joint. By using manual therapy techniques, this joint glide can be restored to significantly improve overall range of motion and function.
Your therapist may use these techniques to improve the mechanics of your joints. Typically, you will be given an exercise program to either stabilize or further mobilize your joint independently in order to create a lasting improvement.
The Functional Movement Screen (FMS) and Selective Functional Movement Assessment (SFMA)
The FMS and SFMA are an evaluative system comprised of seven movement tests that require a balance of both mobility and stability. This is a total body assessment. These patterns are used to assess the quality of movements in the body. Weakness, imbalance, asymmetries and limitations in the movement patterns allow clinicians to treat the weakest link.These systems are very helpful during the initial patient examination and can help guide the clinician to choose the most effective treatment option for the individual to get to the heart of their dysfunction in the quickest manner possible.
Impact Protocol
The extremity team also offers a unique protocol for rehabilitation of our knee patients following surgery. This protocol was developed by one of the co-owners Nathan Lilley and was released by Biomet Sportmedicine in Digital and DVD format in 2007. Impact consists of graded progressive plyometrics beginning at about 8 weeks post-operatively extending to the 4-6 month mark. One of the most controversial and challenging dilemma to the clinician is knowing when to safely progress a patient from standard rehab (ROM ,PRE, Proprioception training, Etc.) into impact and more sport specific training. The purpose of the Impact protocol is to take a research derived criterion-based approach to progressing a patient all the way back to their given sport. This protocol is not for all patients and should only be used for individuals looking to return to competitive athletics. The protocol is outlined in detail under the “Impact: Accelerate Your rehab” tab (please link to this tab)
The following conditions are specialties for this team:
Shoulder Injuries
Impingement Syndrome/Tendinopathy
Rotator Cuff Pathology
Scapular Dyskinesia
Adhesive Capsulitis: Frozen Shoulder
Labral Pathology
Shoulder Instability/Dislocation: Glenohumeral Joint
Total Shoulder Replacement and Reverse Total Shoulder Replacement(TSA, RTSA)
Acromioclavicular Joint Pathology: AC Separation
Shoulder Fractures
Osteoarthritis
Elbow and Wrist
- Tendinopathy/Bursitis: Tennis Elbow, Golfer’s Elbow
- Ulnar Collateral Ligament Injuries
Elbow Fractures
Tendinopathy
Wrist Fractures
Hip Conditions
Femoral Acetabular Impingement (FAI)
Labral Pathology
Osteochondral Injuries (Micro Fracture)
Tendinopathy/Bursitis
Osteoarthritis
Hip Fractures
Hip Pointer
Myositis Ossificans
Hamstring, Groin and Quad Strains
Thigh Contusions
Total Hip Replacement (THA): Posterior and Anterior Approach
Knee Injuries
Patellofemoral Syndrome
ITB Syndrome: Runner’s Knee
Chondromalacia
Osgood Schlaters
Jumper’s Knee
Hyperlateral Patella Pressure Syndrome
Plica Syndrome
Hoffa’s Syndrome
Patella Instability/Dislocation
Tendinopathy/Bursitis
ACL, PCL, MCL, LCL Injuries
Complex Ligament Reconstruction (Knee Dislocation)
Meniscal Pathology
Osteochondral Injuries (Micro Fracture)
Osteoarthritis
Knee Fractures
Total Knee Replacement
Ankle / Lower Leg / Feet
Lateral and Medial Ligament Sprains
Syndesmotic Injuries: High Ankle Sprains
Tendinopathy/Bursitis
Achillles Tendinopathy/Rupture
Ankle Fractures
Calf Strain
Shin Splints
Compartment Syndrome
Total Ankle Replacement/Fusions
Plantar Fascitis